ENT DEPARTMENT
Hearing Loss, Vocal Cord Nodule, Vocal Cord Paralysis, Nasal Polip, Adenoid, Recurrent ear infection, Allergic Rhinitis/Sinusitis
Stories

chronic pancreatitis treatment in hindi
पैंक्रियास ठीक करने के उपाय
पैंक्रियाटाइटिस एक बीमारी है जो आपके पैंक्रियास में हो सकती है। पैंक्रियास आपके पेट में एक लंबी ग्रंथि है जो भोजन को पचाने में आपकी मदद करती है। यह आपके रक्त प्रवाह में हार्मोन भी जारी करता है जो आपके शरीर को ऊर्जा के लिए भोजन का उपयोग करने में मदद करता है। यदि आपका पैंक्रियास क्षतिग्रस्त हो गया है, तो पाचन एंजाइम सामान्य रूप से आपकी छोटी आंत में नहीं जा सकते हैं और आपका शरीर ऊर्जा के लिए भोजन का उपयोग नहीं कर सकता है।
पैंक्रियास शरीर का एक महत्वपूर्ण हिस्सा है जो हार्मोन इंसुलिन का उत्पादन करके रक्त शर्करा को नियंत्रित करने में मदद करता है। यदि इस अंग को नुकसान होता है, तो इससे मानव शरीर में गंभीर समस्याएं हो सकती हैं। ऐसी ही एक समस्या है जब पैंक्रियास में सूजन हो जाती है, जिसे तीव्र पैंक्रियाटाइटिस कहा जाता है।
क्रोनिक पैंक्रियाटाइटिस पैंक्रियास की सूजन है जो लंबे समय तक रह सकती है। इससे पैंक्रियास और अन्य जटिलताओं को स्थायी नुकसान हो सकता है। इस सूजन से निशान ऊतक विकसित हो सकते हैं, जो इंसुलिन उत्पन्न करने वाली कोशिकाओं को नुकसान पहुंचा सकते हैं। यह पुरानी अग्नाशयशोथ वाले लगभग 45 प्रतिशत लोगों में मधुमेह का कारण बन सकता है। भारी शराब का सेवन भी वयस्कों में पैंक्रियाटाइटिस का कारण बन सकता है। ऑटोइम्यून और आनुवंशिक रोग, जैसे सिस्टिक फाइब्रोसिस, कुछ लोगों में पुरानी पैंक्रियाटाइटिस का कारण बन सकते हैं।
उत्तर भारत में, ऐसे बहुत से लोग हैं जिनके पास पीने के लिए बहुत अधिक है और कभी-कभी एक छोटा सा पत्थर उनके पित्ताशय में फंस सकता है और उनके अग्न्याशय के उद्घाटन को अवरुद्ध कर सकता है। इससे उन्हें अपना खाना पचाने में मुश्किल हो सकती है। 3 हाल ही में एशिया-प्रशांत क्षेत्र के विभिन्न देशों में किए गए एक सर्वेक्षण के अनुसार दक्षिण भारत में पुरानी अग्नाशयशोथ की व्यापकता प्रति 100,000 जनसंख्या पर 114-200 मामले हैं।
क्रोनिक पैंक्रियाटाइटिस के लक्षण ?
-कुछ लोगों को पेट में दर्द होता है जो पीठ तक फैल सकता है। -यह दर्द मतली और उल्टी जैसी चीजों के कारण हो सकता है। -खाने के बाद दर्द और बढ़ सकता है। -कभी-कभी किसी के पेट को छूने पर दर्द महसूस हो सकता है। -व्यक्ति को बुखार और ठंड लगना भी हो सकता है। वे बहुत कमजोर और थका हुआ भी महसूस कर सकते हैं।
क्रोनिक पैंक्रियाटाइटिस के कारण ?
-पित्ताशय की पथरी -शराब
-रक्त में उच्च ट्राइग्लिसराइड का स्तर -रक्त में उच्च कैल्शियम का स्तर
होम्योपैथी में क्रोनिक पैंक्रियाटाइटिस का इलाज कैसे किया जाता है?
होम्योपैथी में क्रोनिक पैंक्रियाटाइटिस नेक्रोसिस का उपचार उपचारात्मक है। आप कितने समय तक इस बीमारी से पीड़ित रहेंगे यह काफी हद तक आपकी उपचार योजना पर निर्भर करता है। ब्रह्म अनुसंधान पर आधारित चिकित्सकीय रूप से सिद्ध वैज्ञानिक उपचार मॉड्यूल इस बीमारी के इलाज में अत्यधिक प्रभावी हैं। हमारे पास आपके मामले का व्यवस्थित रूप से निरीक्षण और विश्लेषण करने, सभी संकेतों और लक्षणों, रोग के पाठ्यक्रम का दस्तावेजीकरण करने, रोग के चरण, पूर्वानुमान और जटिलताओं को समझने की क्षमता है, हमारे पास अत्यधिक योग्य डॉक्टरों की एक टीम है। फिर वे आपकी बीमारी के बारे में विस्तार से बताएंगे, आपको एक उचित आहार योजना (क्या खाएं और क्या नहीं खाएं), व्यायाम योजना, जीवनशैली योजना और कई अन्य कारक प्रदान करेंगे जो आपके समग्र स्वास्थ्य में सुधार कर सकते हैं। पढ़ाना। व्यवस्थित उपचार रोग ठीक होने तक होम्योपैथिक औषधियों से उपचार करें। इससे कोई फर्क नहीं पड़ता कि आप कितने समय से बीमारी से पीड़ित हैं, चाहे वह थोड़े समय के लिए हो या कई सालों से। हम सभी ठीक हो सकते हैं, लेकिन बीमारी के प्रारंभिक चरण में हम तेजी से ठीक हो जाते हैं। पुरानी या देर से आने वाली या लंबे समय तक चलने वाली बीमारियों को ठीक होने में अधिक समय लगता है। समझदार लोग इस बीमारी के लक्षण दिखते ही इलाज शुरू कर देते हैं। इसलिए, यदि आपको कोई असामान्यता नज़र आती है, तो कृपया तुरंत हमसे संपर्क करें।
Acute Necrotizing pancreas treatment in hindi
तीव्र नेक्रोटाइज़िंग अग्नाशयशोथ ?
आक्रामक अंतःशिरा द्रव पुनर्जीवन, दर्द प्रबंधन, और आंत्र भोजन की जल्द से जल्द संभव शुरुआत उपचार के मुख्य घटक हैं। जबकि उपरोक्त सावधानियों से बाँझ परिगलन में सुधार हो सकता है, संक्रमित परिगलन के लिए अतिरिक्त उपचार की आवश्यकता होती है।
तीव्र नेक्रोटाइज़िंग अग्नाशयशोथ के लक्षण ? - बुखार - फूला हुआ पेट - मतली और दस्त तीव्र नेक्रोटाइज़िंग अग्नाशयशोथ के कारण ?
- अग्न्याशय में चोट - उच्च रक्त कैल्शियम स्तर और रक्त वसा सांद्रता
ऐसी स्थितियाँ जो अग्न्याशय को प्रभावित करती हैं और आपके परिवार में चलती रहती हैं, उनमें सिस्टिक फाइब्रोसिस और अन्य आनुवंशिक विकार शामिल हैं जिनके परिणामस्वरूप बार-बार अग्नाशयशोथ होता है|
क्या एक्यूट नेक्रोटाइज़िंग पैंक्रिएटाइटिस का इलाज होम्योपैथी से संभव है ?
हां, होम्योपैथिक उपचार चुनकर एक्यूट नेक्रोटाइज़िंग पैन्क्रियाटाइटिस का इलाज संभव है। होम्योपैथिक उपचार चुनने से आपको इन दवाओं का कोई साइड इफेक्ट नहीं होगा और यह समस्या को जड़ से खत्म कर देता है, इसीलिए आपको अपने एक्यूट नेक्रोटाइज़िंग पैन्क्रियाटाइटिस के इलाज के लिए होम्योपैथिक उपचार का ही चयन करना चाहिए।
आप तीव्र नेक्रोटाइज़िंग अग्नाशयशोथ से कैसे छुटकारा पा सकते हैं ?
शुरुआती चरण में सर्वोत्तम उपचार चुनने से आपको एक्यूट नेक्रोटाइज़िंग पैन्क्रियाटाइटिस से छुटकारा मिल जाएगा। होम्योपैथिक उपचार का चयन करके, ब्रह्म होम्योपैथी आपको एक्यूट नेक्रोटाइज़िंग पैन्क्रियाटाइटिस के लिए सबसे विश्वसनीय उपचार देना सुनिश्चित करता है। एक्यूट नेक्रोटाइज़िंग पैन्क्रियाटाइटिस के लिए होम्योपैथिक उपचार सबसे अच्छा इलाज है। जैसे ही आप एक्यूट नेक्रोटाइज़िंग पैन्क्रियाटाइटिस को ठीक करने के लिए अपना उपचार शुरू करेंगे, आपको निश्चित परिणाम मिलेंगे।
होम्योपैथिक उपचार से तीव्र नेक्रोटाइज़िंग अग्नाशयशोथ का इलाज संभव है। आप कितने समय से बीमारी से पीड़ित हैं, इसका उपचार योजना पर बहुत प्रभाव पड़ता है। इससे कोई फर्क नहीं पड़ता कि आप कब से अपनी बीमारी से पीड़ित हैं, या तो हाल ही में या कई वर्षों से - हमारे पास सब कुछ ठीक है, लेकिन बीमारी के शुरुआती चरण में, आप तेजी से ठीक हो जाएंगे। पुरानी स्थितियों के लिए या बाद के चरण में या कई वर्षों की पीड़ा के मामले में, इसे ठीक होने में अधिक समय लगेगा। बुद्धिमान व्यक्ति हमेशा इस बीमारी के किसी भी लक्षण को देखते ही तुरंत इलाज शुरू कर देते हैं, इसलिए जैसे ही आपमें कोई असामान्यता दिखे तो तुरंत हमसे संपर्क करें।
ब्रह्म होम्योपैथिक हीलिंग एवं रिसर्च सेंटर की उपचार योजना
ब्रह्म अनुसंधान आधारित, चिकित्सकीय रूप से प्रमाणित, वैज्ञानिक उपचार मॉड्यूल इस बीमारी को ठीक करने में बहुत प्रभावी है। हमारे पास सुयोग्य डॉक्टरों की एक टीम है जो आपके मामले का व्यवस्थित रूप से निरीक्षण और विश्लेषण करती है, रोग की प्रगति के साथ-साथ सभी संकेतों और लक्षणों को रिकॉर्ड करती है, इसकी प्रगति के चरणों, पूर्वानुमान और इसकी जटिलताओं को समझती है। उसके बाद वे आपको आपकी बीमारी के बारे में विस्तार से बताते हैं, आपको उचित आहार चार्ट [क्या खाएं या क्या न खाएं], व्यायाम योजना, जीवन शैली योजना प्रदान करते हैं और कई अन्य कारकों के बारे में मार्गदर्शन करते हैं जो व्यवस्थित प्रबंधन के साथ आपकी सामान्य स्वास्थ्य स्थिति में सुधार कर सकते हैं। जब तक यह ठीक न हो जाए तब तक होम्योपैथिक दवाओं से अपनी बीमारी का इलाज करें।
तीव्र नेक्रोटाइज़िंग अग्नाशयशोथ के लिए आहार ?
कुपोषण और पोषण संबंधी कमियों को रोकने के लिए, सामान्य रक्त शर्करा के स्तर को बनाए रखने और मधुमेह, गुर्दे की समस्याओं और पुरानी अग्नाशयशोथ से जुड़ी अन्य स्थितियों को रोकने या बेहतर ढंग से प्रबंधित करने के लिए, अग्नाशयशोथ की तीव्र घटना से बचना महत्वपूर्ण है।
यदि आप एक स्वस्थ आहार योजना की तलाश में हैं, तो ब्रह्म होम्योपैथी से संपर्क करें। हमारे विशेषज्ञ आपकी व्यक्तिगत आवश्यकताओं के अनुरूप एक योजना बनाने में आपकी सहायता कर सकते हैं

Pancreatitis treatment in hindi
पैंक्रियाटाइटिस ?
जब पैंक्रियाटाइटिसमें सूजन और संक्रमण हो जाता है तो इससे पैंक्रिअटिटिस नामक रोग हो जाता है। पैंक्रियास एक लंबा, चपटा अंग है जो पेट के पीछे पेट के शीर्ष पर छिपा होता है। पैंक्रिअटिटिस उत्तेजनाओं और हार्मोन का उत्पादन करके पाचन में मदद करता है जो आपके शरीर में ग्लूकोज के प्रसंस्करण को विनियमित करने में मदद करते हैं।
पैंक्रियाटाइटिस के लक्षण:
-पेट के ऊपरी भाग में दर्द होना। -बेकार वजन घटाना. -पेट का ख़राब होना.
-शरीर का असामान्य रूप से उच्च तापमान। -पेट को छूने पर दर्द होना। -तेज़ दिल की धड़कन. -हाइपरटोनिक निर्जलीकरण.
पैंक्रियाटाइटिस के कारण:
-पित्ताशय में पथरी. -भारी शराब का सेवन.
-भारी खुराक वाली दवाएँ। -हार्मोन का असंतुलन. -रक्त में वसा जो ट्राइग्लिसराइड्स का कारण बनता है। -आनुवंशिकता की स्थितियाँ. -पेट में सूजन ।
क्या होम्योपैथी पैंक्रियाटाइटिस को ठीक कर सकती है?
हाँ, होम्योपैथीपैंक्रियाटाइटिसको ठीक कर सकती है। ब्रह्म होम्योपैथी आपको पैंक्रिअटिटिस के लिए सबसे भरोसेमंद उपचार देना सुनिश्चित करती है।
पैंक्रियाटाइटिस के लिए सबसे अच्छा उपचार क्या है?
यदि पैंक्रियाज अच्छी तरह से काम नहीं कर रहा है तो होम्योपैथिक उपचार वास्तव में बेहतर होने में मदद करने का एक अच्छा तरीका है। जब आप उपचार शुरू करते हैं, तो आप जल्दी परिणाम देखेंगे। बहुत सारे लोग इस इलाज के लिए ब्रह्म होम्योपैथी जा रहे हैं और वे वास्तव में अच्छा कर रहे हैं। ब्रह्म होम्योपैथी आपके पैंक्रियाज के को बेहतर बनाने में मदद करने के लिए आपको सबसे तेज़ और सुरक्षित तरीका प्रदान करना सुनिश्चित करती है।
ब्रह्म होम्योपैथिक हीलिंग एंड रिसर्च सेंटर की उपचार योजना
बीमार होने पर लोगों को बेहतर महसूस कराने में मदद करने के लिए हमारे पास एक विशेष तरीका है। हमारे पास वास्तव में स्मार्ट डॉक्टर हैं जो ध्यान से देखते हैं और नोट करते हैं कि बीमारी व्यक्ति को कैसे प्रभावित कर रही है। फिर, वे सलाह देते हैं कि क्या खाना चाहिए, व्यायाम करना चाहिए और स्वस्थ जीवन कैसे जीना चाहिए। वे व्यक्ति को ठीक होने में मदद करने के लिए विशेष दवा भी देते हैं। यह तरीका कारगर साबित हुआ है!
Tips

mirgi aane par kya tip ko follow kre?
१) मिर्गी के लिए उपयोगी सुझाव
मिर्गी न्यूरोलॉजिकल बीमारी है, जिस में मस्तिष्क की विद्युत गतिविधि असामान्य हो जाती है, जिससे बार-बार दौरे पड़ सकते हैं।
- यह किसी भी उम्र के व्यक्ति को प्रभावित कर सकती है। सही उपचार, नियमित दवाओं और स्वस्थ जीवनशैली के माध्यम से मिर्गी से पीड़ित व्यक्ति सामान्य और सक्रिय जीवन जी सकता है।
२) मिर्गी क्या हैमिर्गी ऐसी स्थिति है, जिस में व्यक्ति को बार-बार दौरे आते हैं। दौरे कई प्रकार के हो सकते हैं। कुछ लोगों में पूरे शरीर में झटके आते हैं, जबकि कुछ लोगों में कुछ सेकंड के लिए ध्यान भटक जाता है या वे एक जगह स्थिर हो जाते हैं। - मिर्गी का कारण सिर की चोट, जन्म के समय मस्तिष्क की समस्या, संक्रमण, आनुवंशिक कारण या अन्य न्यूरोलॉजिकल विकार हो सकते हैं।
३) मिर्गी के रोगियों के लिए महत्वपूर्ण सुझाव
1. दवा को नियमित रूप से लें
- मिर्गी के उपचार में डॉक्टर द्वारा दी गई दवाओं का नियमित सेवन महत्वपूर्ण है।
- दवा भूलना या बिना डॉक्टर की सलाह के बंद करना दौरे आने का जोखिम बढ़ा सकता है। इसलिए दवाएं हमेशा निर्धारित समय पर लें.
2. सही नींद लें
- नींद की कमी मिर्गी के दौरे को ट्रिगर कर सकती है। वयस्कों को प्रतिदिन 7 से 9 घंटे की नींद लेने का प्रयास करना चाहिए।
3. तनाव को नियंत्रित करें 4. स्वस्थ और संतुलित आहार अपनाएं
- पौष्टिक भोजन शरीर और मस्तिष्क दोनों के लिए आवश्यक है। ताजे फल, हरी सब्जियां, साबुत अनाज, प्रोटीन और पर्याप्त पानी का सेवन करें।
5. शराब और नशीले पदार्थों से बचें 6. संभावित ट्रिगर्स को पहचानें
- कुछ लोगों में तेज चमकती रोशनी, अत्यधिक थकान, तनाव, बुखार या नींद की कमी दौरे को बढ़ा सकते हैं।
7. सुरक्षा का ध्यान रखें
- यदि आप को मिर्गी है, तो तैराकी, ऊंचाई पर काम करने या भारी मशीन चलाने जैसी गतिविधियों में सावधानी बरतें।
8. परिवार और मित्रों को जानकारी दें
४) दौरा आने पर क्या करें- सुरक्षित स्थान पर लिटाएं। - उसके सिर के नीचे मुलायम वस्तु रखें।- आसपास की खतरनाक वस्तुएं हटा दें।- व्यक्ति को करवट दिलाने की कोशिश करें।- दौरे का समय नोट करें।- यदि दौरा 5 मिनट से अधिक चले या लगातार कई दौरे आएं, तो तुरंत चिकित्सा सहायता लें।
Gout ke liye kya tip ko follow kre?
Gout (गाउट) के लिए उपयोगी टिप्स
गाउट एक प्रकार का गठिया (Arthritis) है, जो शरीर में यूरिक एसिड (Uric Acid) की मात्रा बढ़ जाने के कारण होता है। जब यूरिक एसिड के छोटे-छोटे क्रिस्टल जोड़ों में जमा हो जाते हैं, तो तेज दर्द, सूजन और लालिमा पैदा होती है। यह समस्या अक्सर पैर के अंगूठे, टखनों, घुटनों और अन्य जोड़ों को प्रभावित करती है। सही खान-पान, जीवनशैली में बदलाव और नियमित चिकित्सा देखभाल से गाउट को काफी हद तक नियंत्रित किया जा सकता है।
१) गाउट के मुख्य कारण
गाउट का प्रमुख कारण रक्त में यूरिक एसिड का बढ़ना है। यह स्थिति तब होती है जब शरीर अधिक यूरिक एसिड बनाता है या किडनी इसे पर्याप्त मात्रा में बाहर नहीं निकाल पाती। लाल मांस, अंगों का मांस, कुछ समुद्री खाद्य पदार्थ, अत्यधिक शराब और मीठे पेय पदार्थ यूरिक एसिड बढ़ाने में योगदान दे सकते हैं। मोटापा, मधुमेह, उच्च रक्तचाप और पारिवारिक इतिहास भी जोखिम बढ़ाते हैं।
२) गाउट को नियंत्रित करने के लिए महत्वपूर्ण टिप्स
1. पर्याप्त पानी पिएं पानी शरीर से अतिरिक्त यूरिक एसिड को बाहर निकालने में मदद करता है। प्रतिदिन 2–3 लीटर पानी पीने का प्रयास करें, जब तक कि आपके डॉक्टर ने किसी अन्य कारण से तरल पदार्थ सीमित करने की सलाह न दी हो। अच्छी हाइड्रेशन गाउट अटैक की संभावना कम कर सकती है। 2. कम प्यूरिन वाला आहार अपनाएं प्यूरिन ऐसे पदार्थ हैं जो शरीर में टूटकर यूरिक एसिड बनाते हैं। गाउट के मरीजों को निम्न खाद्य पदार्थों का सेवन सीमित करना चाहिए
लाल मांस (मटन, बीफ आदि) लीवर और अन्य अंगों का मांस सार्डिन, एन्कोवी और कुछ अन्य समुद्री मछलियां अत्यधिक प्रोसेस्ड मांस इसके बजाय सब्जियां, फल, साबुत अनाज और कम वसा वाले डेयरी उत्पादों को प्राथमिकता दें। 3. मीठे पेय पदार्थों से बचें फ्रुक्टोज युक्त सॉफ्ट ड्रिंक्स और पैकेज्ड जूस यूरिक एसिड बढ़ा सकते हैं। इनके स्थान पर सादा पानी, नींबू पानी (बिना अधिक चीनी) और नारियल पानी का सेवन बेहतर विकल्प हो सकता है। 4. वजन नियंत्रित रखें अधिक वजन होने से गाउट का खतरा बढ़ जाता है। संतुलित आहार और नियमित व्यायाम के माध्यम से धीरे-धीरे वजन कम करना फायदेमंद हो सकता है। हालांकि, बहुत तेजी से वजन घटाने की कोशिश न करें, क्योंकि इससे यूरिक एसिड अस्थायी रूप से बढ़ सकता है। 5. शराब का सेवन सीमित करें विशेष रूप से बीयर और अधिक मात्रा में शराब का सेवन गाउट अटैक को ट्रिगर कर सकता है। यदि आपको बार-बार गाउट की समस्या होती है, तो शराब से परहेज करना बेहतर हो सकता है। 6. नियमित व्यायाम करें हल्की से मध्यम शारीरिक गतिविधियां जैसे पैदल चलना, योग और साइक्लिंग संपूर्ण स्वास्थ्य के लिए लाभदायक हैं। नियमित व्यायाम वजन नियंत्रण में मदद करता है और कई अन्य बीमारियों के जोखिम को कम करता है। 7. डॉक्टर द्वारा दी गई दवाएं नियमित लें
यदि डॉक्टर ने यूरिक एसिड कम करने या गाउट नियंत्रित करने की दवा दी है, तो उसे नियमित रूप से लें। बिना चिकित्सकीय सलाह के दवा बंद न करें। नियमित जांच के माध्यम से यूरिक एसिड स्तर की निगरानी भी आवश्यक है।
३) गाउट अटैक के दौरान क्या करें
- प्रभावित जोड़ को आराम दें।
- सूजन कम करने के लिए बर्फ की सिकाई करें। - पर्याप्त पानी पिएं। - डॉक्टर द्वारा सुझाई गई दवा समय पर लें।
- दर्द बहुत अधिक होने या बार-बार अटैक आने पर तुरंत चिकित्सक से संपर्क करें।
४) किन खाद्य पदार्थों का सेवन बढ़ाएं
कुछ खाद्य पदार्थ गाउट रोगियों के लिए लाभदायक माने जाते हैं - चेरी और अन्य रंगीन फल - कम वसा वाला दूध और दही - हरी सब्जियां - साबुत अनाज - बादाम और अखरोट - विटामिन C से भरपूर फल जैसे संतरा और अमरूद
osteoporosis kya hai? kis ke karan se hota hai?
१) ऑस्टियोपोरोसिस क्या है
यह ऐसी स्थिति है, जिस में हड्डियाँ कमजोर और भुरभुरी हो जाती हैं। इस से मामूली चोट या गिरने पर भी फ्रैक्चर होने का खतरा बढ़ जाता है - यह समस्या विशेष रूप से बढ़ती उम्र के लोगों, महिलाओं और कैल्शियम की कमी वाले व्यक्तियों में देखी जाती है। सही खानपान, नियमित व्यायाम और स्वस्थ जीवनशैली से ऑस्टियोपोरोसिस के जोखिम को कम किया जा सकता है।
1. कैल्शियम युक्त आहार को लें- हड्डियों को मजबूत बनाने के लिए कैल्शियम महत्वपूर्ण पोषक तत्वों में से एक है। - रोज़ाना पर्याप्त मात्रा में कैल्शियम लेना आवश्यक है। दूध, दही, पनीर, छाछ,बादाम और हरी पत्तेदार सब्जियाँ कैल्शियम के अच्छे स्रोत हैं। 2. विटामिन D का महत्व
-प्रतिदिन सुबह की धूप में 15–20 मिनट बैठना या टहलना विटामिन D प्राप्त करने का अच्छा तरीका है।
3. नियमित व्यायाम - हड्डियों को मजबूती बनाए रखने के लिए नियमित शारीरिक गतिविधि आवश्यक है।
- तेज़ चलना, सीढ़ियाँ चढ़ना, योग, हल्का दौड़ना और शक्ति बढ़ाने वाले व्यायाम हड्डियों को मजबूत बनाने में मदद करते हैं।
4. धूम्रपान तथा शराब करने से बचे.
5. संतुलित वजन को बनाए रखें
- बहुत कम वजन वाले लोगों में ऑस्टियोपोरोसिस का जोखिम अधिक होता है।
6. गिरने से बचाव करें - घर में फिसलन वाले फर्श, ढीले कालीन और खराब रोशनी जैसी समस्याओं को दूर करें। 7. सही तरह का प्रोटीन लें
8. नियमित स्वास्थ्य जांच कराएं- आप की उम्र 50 वर्ष से अधिक है, परिवार में ऑस्टियोपोरोसिस का इतिहास है, फ्रैक्चर हो चुका है, तो हड्डियों की घनत्व (Bone Density) जांच करवाना लाभदायक हो सकता है।
9. दवाओं का सेवन केवल डॉ. सलाह के अनुसार करें।
Testimonials

body weakness treatment
ब्रह्म होम्योपैथी से 10 महीने में चमत्कारी इलाज: एक मरीज की कहानी
आज के समय में जब लोग तरह-तरह की बीमारियों से जूझ रहे हैं, तब होम्योपैथी चिकित्सा कई मरीजों के लिए आशा की किरण बन रही है। ऐसी ही एक प्रेरणादायक कहानी है एक मरीज की, जिसने ब्रह्म होम्योपैथी के माध्यम से 10 महीने में अपनी बीमारी से निजात पाई।
शुरुआत में थी थकान और शरीर में भारीपन
मरीज ने बताया, "मुझे कई दिनों से शरीर में थकान, भारीपन और बेचैनी महसूस हो रही थी। यह परेशानी धीरे-धीरे इतनी बढ़ गई कि रोजमर्रा के काम भी कठिन लगने लगे। मेरी माँ पहले से ही ब्रह्म होम्योपैथी क्लीनिक में इलाज करा रही थीं। उन्होंने बताया कि उन्हें वेरीकोज वेन्स की समस्या थी और यहाँ के इलाज से उन्हें बहुत लाभ हुआ था। उनकी सलाह पर मैं भी यहाँ आया।"
होम्योपैथी इलाज का असर मात्र एक सप्ताह में
मरीज के अनुसार, "जब मैंने ब्रह्म होम्योपैथी में डॉक्टर प्रदीप कुशवाहा से परामर्श लिया और उनकी सलाह के अनुसार दवाएं लेना शुरू किया, तो सिर्फ एक हफ्ते के भीतर ही मुझे सुधार महसूस होने लगा। मेरी थकान कम हो गई, शरीर की ऊर्जा बढ़ने लगी और पहले की तुलना में मैं ज्यादा सक्रिय महसूस करने लगा।"
लगातार 10 महीने तक किया उपचार, मिली पूरी राहत
मरीज ने लगातार 10 महीने तक ब्रह्म होम्योपैथी की दवाएं लीं और सभी निर्देशों का पालन किया। उन्होंने कहा, "लगभग 15 दिनों के अंदर ही मेरी स्थिति में काफी सुधार हुआ और अब 10 महीने बाद मैं पूरी तरह स्वस्थ महसूस कर रहा हूँ। यह सब डॉक्टर प्रदीप कुशवाहा और ब्रह्म होम्योपैथी की दवाओं की वजह से संभव हुआ।"
होम्योपैथी: सभी बीमारियों के लिए वरदान
मरीज ने आगे कहा, "इस क्लिनिक का माहौल बहुत अच्छा है और इलाज का तरीका बेहद प्रभावी है। यहाँ की दवाएँ बहुत असरदार हैं और मुझे इनके इस्तेमाल से कोई साइड इफेक्ट भी नहीं हुआ। यह सच में होम्योपैथी का सबसे बेहतरीन केंद्र है। मैं सभी मरीजों से अनुरोध करूंगा कि अगर वे किसी पुरानी बीमारी से परेशान हैं, तो एक बार ब्रह्म होम्योपैथी का इलाज जरूर लें। यह एक बीमार मरीजों के लिए किसी स्वर्ग से कम नहीं है।"
निष्कर्ष
इस मरीज की कहानी यह साबित करती है कि सही चिकित्सा और सही मार्गदर्शन से कोई भी बीमारी ठीक हो सकती है। ब्रह्म होम्योपैथी में न केवल आधुनिक चिकित्सा पद्धति का समावेश है, बल्कि यहाँ मरीजों की समस्याओं को गहराई से समझकर उनका संपूर्ण इलाज किया जाता है। यदि आप भी किसी स्वास्थ्य समस्या से जूझ रहे हैं, तो ब्रह्म होम्योपैथी एक बेहतरीन विकल्प हो सकता है।

acute pancreatitis ka ilaaj
ब्रह्म होम्योपैथी: एक मरीज की जीवन बदलने वाली कहानी
एक्यूट पैन्क्रियाटाइटिस: एक गंभीर समस्या
एक्यूट पैन्क्रियाटाइटिस एक ऐसी स्थिति है जिसमें अग्न्याशय में तीव्र सूजन हो जाती है। जब यह समस्या उत्पन्न होती है, तो मरीज को शुरुआत में इसकी जानकारी नहीं होती, लेकिन दर्द इतना असहनीय होता है कि उसे तुरंत अस्पताल में भर्ती होने की आवश्यकता पड़ती है। इस स्थिति का मुख्य कारण अनुचित जीवनशैली, जंक फूड, शराब का सेवन, ऑटोइम्यून बीमारियां, कुछ रसायन और विकिरण हो सकते हैं। यदि समय रहते सही इलाज नहीं किया गया, तो यह स्थिति क्रॉनिक पैन्क्रियाटाइटिस में बदल सकती है।
अमन बाजपेई की प्रेरणादायक यात्रा
मैं, अमन बाजपेई, पिछले 1.5 वर्षों से एक्यूट पैन्क्रियाटाइटिस का मरीज था। यह समय मेरे लिए बेहद कठिन था। मैं बहुत परेशान था, खाना खाने तक के लिए तरस गया था। पिछले 7-8 महीनों में मैंने रोटी तक नहीं खाई, केवल खिचड़ी और फल खाकर गुजारा कर रहा था। बार-बार मुझे इस बीमारी के हमले झेलने पड़ रहे थे। हर 5-10 दिनों में दवा लेनी पड़ती थी, लेकिन कोई लाभ नहीं हो रहा था।
इस बीमारी के इलाज में मैंने 6-7 लाख रुपये खर्च कर दिए। दिल्ली और झांसी समेत कई बड़े अस्पतालों में इलाज कराया, लेकिन कोई राहत नहीं मिली। मेरा वजन 95 किलो से घटकर 55 किलो हो गया और मैं बहुत कमजोर हो गया था। तभी मुझे सोशल मीडिया के माध्यम से ब्रह्म होम्योपैथी के बारे में पता चला।
ब्रह्म होम्योपैथी: उम्मीद की एक नई किरण
ब्रह्म होम्योपैथी वह जगह है जहां कम खर्च में उत्कृष्ट इलाज संभव है। मैंने आज तक किसी भी डॉक्टर या अस्पताल में इतना अच्छा व्यवहार नहीं देखा। डॉ. प्रदीप कुशवाहा सर ने मुझे एक नई जिंदगी दी। पहले मुझे लगा था कि मैं शायद कभी ठीक नहीं हो पाऊंगा, लेकिन आज मैं पूरी तरह स्वस्थ हूं।
मैं सभी मरीजों को यही सलाह दूंगा कि वे पैसे की बर्बादी न करें और सही इलाज के लिए ब्रह्म होम्योपैथी जाएं। यह भारत में एक्यूट पैन्क्रियाटाइटिस के लिए सबसे अच्छा अस्पताल है। मेरे लिए डॉ. प्रदीप कुशवाहा किसी देवता से कम नहीं हैं।
वैज्ञानिक रूप से प्रमाणित उपचार पद्धति
ब्रह्म होम्योपैथी के विशेषज्ञों ने शोध आधारित एक विशेष उपचार पद्धति विकसित की है, जिससे न केवल लक्षणों में सुधार होता है बल्कि बीमारी को जड़ से ठीक किया जाता है। हजारों मरीज इस उपचार का लाभ ले रहे हैं और उनकी मेडिकल रिपोर्ट में भी उल्लेखनीय सुधार देखा गया है।
यदि आप भी इस बीमारी से जूझ रहे हैं और सही इलाज की तलाश कर रहे हैं, तो ब्रह्म होम्योपैथी से संपर्क करें। यह न केवल बीमारी को बढ़ने से रोकता है बल्कि इसे जड़ से ठीक भी करता है।

urticaria ka ilaaj
रेणुका बहन श्रीमाली की प्रेरणादायक कहानी: 10 साल की तकलीफ से छुटकारारेणुका बहन श्रीमाली पिछले 10 वर्षों से एक गंभीर समस्या से जूझ रही थीं। उन्हें जब भी कुछ खाने की कोशिश करतीं, उनका शरीर फूल जाता था और अत्यधिक खुजली होने लगती थी। इस समस्या के कारण वे बहुत परेशान थीं और 10 वर्षों तक कुछ भी सही तरीके से नहीं खा पाती थीं। उन्होंने कई जगहों पर इलाज कराया, लेकिन कोई भी उपचार कारगर नहीं हुआ।
ब्रह्म होम्योपैथिक रिसर्च सेंटर से नई उम्मीदआखिरकार, 17 मई 2021 को उन्होंने ब्रह्म होम्योपैथिक रिसर्च सेंटर में अपना ट्रीटमेंट शुरू किया। पहले से निराश हो चुकीं रेणुका बहन के लिए यह एक नई उम्मीद की किरण थी।एक साल में चमत्कारी सुधारट्रीटमेंट शुरू करने के बाद, धीरे-धीरे उनके स्वास्थ्य में सुधार होने लगा। एक साल के भीतर उन्होंने अपने आहार में वे सभी चीजें फिर से शुरू कर दीं, जिन्हें वे पहले नहीं खा पाती थीं। पहले जहाँ कोई भी चीज खाने से उनका शरीर फूल जाता था और खुजली होती थी, वहीं अब वे बिना किसी परेशानी के सामान्य जीवन जी रही हैं।ब्रह्म होम्योपैथिक रिसर्च सेंटर का योगदान
रेणुका बहन का कहना है कि यह इलाज उनके लिए किसी चमत्कार से कम नहीं था। उन्होंने अपनी पुरानी जीवनशैली को फिर से अपनाया और अब वे पूरी तरह से स्वस्थ महसूस कर रही हैं। उनके अनुसार, ब्रह्म होम्योपैथिक रिसर्च सेंटर में इलाज का असर तुरंत दिखने लगता है और दवाइयाँ भी पूरी तरह से प्रभावी होती हैं।
अन्य समस्याओं के लिए भी कारगर
इस रिसर्च सेंटर में सिर्फ एलर्जी ही नहीं, बल्कि स्पॉन्डिलाइटिस, पीसीओडी जैसी कई अन्य बीमारियों का भी सफलतापूर्वक इलाज किया जाता है। रेणुका बहन जैसी कई अन्य मरीजों को भी यहाँ से सकारात्मक परिणाम मिले हैं।
रेणुका बहन का संदेश
रेणुका बहन उन सभी लोगों को धन्यवाद देती हैं जिन्होंने उनके इलाज में मदद की। वे यह संदेश देना चाहती हैं कि यदि कोई भी व्यक्ति किसी पुरानी बीमारी से परेशान है और अब तक उसे कोई समाधान नहीं मिला है, तो उन्हें ब्रह्म होम्योपैथिक रिसर्च सेंटर में एक बार अवश्य आना चाहिए।
"यहाँ इलाज प्रभावी, सुरक्षित और प्राकृतिक तरीके से किया जाता है। मैं इस सेंटर के प्रति आभार व्यक्त करती हूँ, जिसने मुझे 10 साल पुरानी तकलीफ से राहत दिलाई।"
अगर आप भी किसी स्वास्थ्य समस्या से जूझ रहे हैं और समाधान की तलाश में हैं, तो इस होम्योपैथिक उपचार को आज़मा सकते हैं।
Departments
brahm homeopathy medicine tracking details
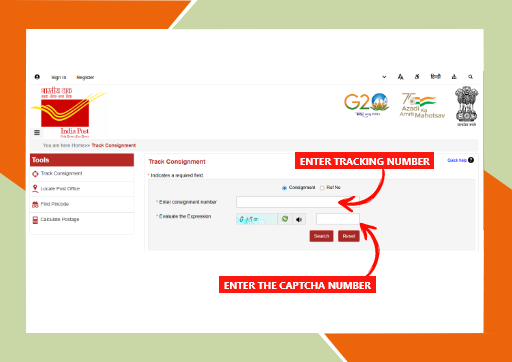
ब्रह्म होम्योपैथी मेडिसिन ट्रैकिंग कैसे करें?
अगर आपने ब्रह्म होम्योपैथी से दवा ऑर्डर की है और आप उसकी डिलीवरी की स्थिति जानना चाहते हैं, तो आप आसानी से इंडिया पोस्ट की वेबसाइट पर जाकर अपनी दवा को ट्रैक कर सकते हैं।
- ब्रह्म होम्योपैथी अधिकतर दवाएं भारत सरकार की इंडिया पोस्ट सेवा के माध्यम से भेजता है, जिसमें हर पार्सल का एक यूनिक ट्रैकिंग नंबर होता है।
Brahm Homeopathy Medicine Tracking Details.
- ट्रैकिंग के लिए सबसे पहले India Post की वेबसाइट पर जाएं। वहां “Track Consignment” विकल्प पर क्लिक करें। इसके बाद स्क्रीन पर दिख रही जगह पर अपना ट्रैकिंग नंबर डालें जो आपको ब्रह्म होम्योपैथी से SMS या Email के माध्यम से मिला होगा। - फिर स्क्रीन पर दिखाई दे रही कैप्चा कोड को सही-सही भरें और “Search” बटन पर क्लिक करें।
- इसके बाद आपको आपकी दवा का पूरा स्टेटस दिखेगा – जैसे कि पार्सल कहां पहुंचा है, कब डिलीवर होगा आदि। यह प्रक्रिया सरल है और घर बैठे आप अपने ऑर्डर की जानकारी आसानी से प्राप्त कर सकते हैं।
इस प्रकार, ब्रह्म होम्योपैथी की ट्रैकिंग सुविधा पारदर्शिता और भरोसेमंद सेवा का परिचायक है।

ENT DEPARTMENT
Hearing Loss, Vocal Cord Nodule, Vocal Cord Paralysis, Nasal Polip, Adenoid, Recurrent ear infection, Allergic Rhinitis/Sinusitis

GENERAL MEDICINE
Diabetes
Hypertension
Thyroid Disorders
Cholesterol problem (Dislipimidia)
Diseases
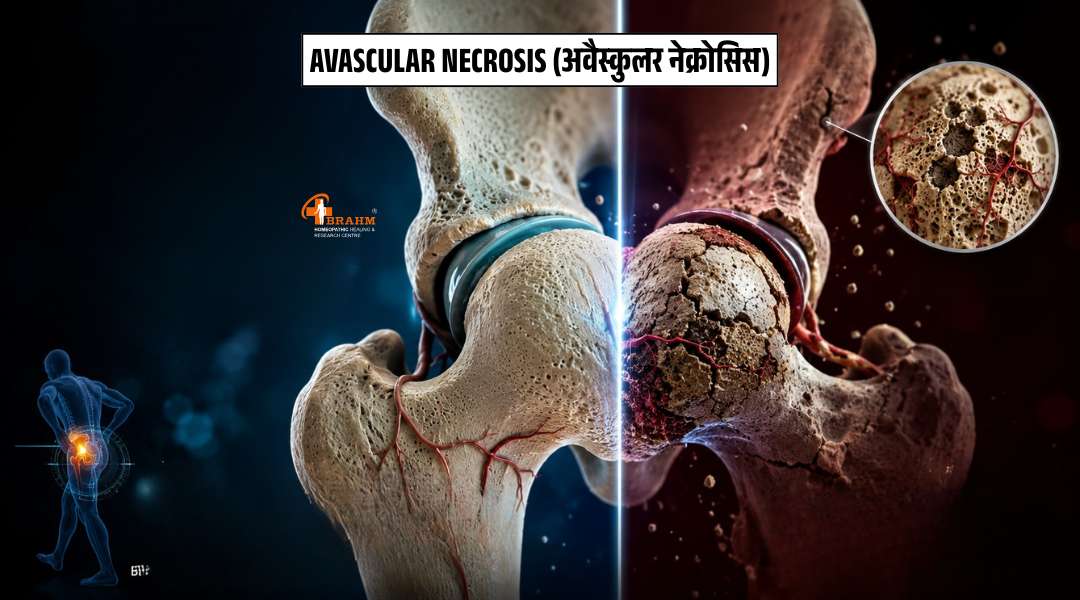
avn ka homeopathy me ilaj?
Avascular Necrosis (अवैस्कुलर नेक्रोसिस) यह बीमारी क्या है?अवैस्कुलर नेक्रोसिस (AVN) एक गंभीर हड्डी की बीमारी है जिसमें हड्डी तक रक्त की आपूर्ति बंद हो जाती है। रक्त न मिलने से हड्डी की कोशिकाएं मरने लगती हैं और हड्डी धीरे-धीरे नष्ट होने लगती है। यह सबसे अधिक कूल्हे की हड्डी (Hip Joint) में होती है लेकिन घुटने, कंधे और जबड़े की हड्डी में भी हो सकती है। इसे Osteonecrosis भी कहते हैं। यह बीमारी कैसे होती है?हड्डियों को जीवित रहने के लिए निरंतर रक्त की आपूर्ति जरूरी है। जब किसी कारण से रक्त वाहिकाएं संकरी हो जाती हैं या बंद हो जाती हैं तो हड्डी को ऑक्सीजन और पोषण नहीं मिलता। इससे पहले हड्डी कमजोर होती है फिर टूटने लगती है और अंत में जोड़ पूरी तरह खराब हो जाता है।
बीमारी के कारण (Causes)?- स्टेरॉयड दवाओं का लंबे समय तक उपयोग — सबसे बड़ा कारण- शराब का अत्यधिक सेवन- हड्डी में चोट या फ्रैक्चर- सिकल सेल एनीमिया- रेडिएशन थेरेपी
लक्षण (Symptoms)?- शुरुआत में कोई लक्षण नहीं- धीरे-धीरे कूल्हे, जांघ या घुटने में दर्द- चलने पर दर्द बढ़ना- जोड़ों में अकड़न- लंगड़ाकर चलना- लेटने पर भी दर्द रहना- जोड़ की गति सीमित होना- उन्नत अवस्था में जोड़ का पूरी तरह खराब होनादर्द अचानक तेज हो सकता है क्या खाएं?- विटामिन D — धूप में बैठें और मछली खाएं- हरी सब्जियां — पालक, ब्रोकली- अखरोट और बादाम — हड्डियों के लिए फायदेमंद- तिल — कैल्शियम का अच्छा स्रोत- आंवला और संतरा — विटामिन C हड्डियों को मजबूत करता है- अलसी के बीज — ओमेगा 3 सूजन कम करता है- हल्दी वाला दूध — हड्डियों की सूजन में राहत- दालें और फलियां — प्रोटीन के लिए क्या न खाएं?- शराब बिल्कुल बंद करें- धूम्रपान पूरी तरह बंद करें- स्टेरॉयड दवाएं बिना डॉक्टर की सलाह के न लें- अधिक नमक — हड्डियों से कैल्शियम निकालता है- कोल्ड ड्रिंक और सोडा — हड्डियां कमजोर करता है- अधिक कैफीन- तला-भुना और जंक फूड- प्रोसेस्ड और डिब्बाबंद खाना

Ankylosing Spondylitis ke kya laksan hote hai?
Ankylosing Spondylitis (एंकिलोजिंग स्पॉन्डिलाइटिस) यह बीमारी क्या है?एंकिलोजिंग स्पॉन्डिलाइटिस रीढ़ की हड्डी (Spine) की एक दीर्घकालिक सूजन संबंधी बीमारी है। इसमें रीढ़ की हड्डियों के बीच के जोड़ों में सूजन आती है और धीरे-धीरे वे आपस में जुड़ने लगते हैं। इससे रीढ़ की हड्डी कठोर और अनम्य हो जाती है। यह एक ऑटोइम्यून बीमारी है जो पुरुषों में महिलाओं की तुलना में अधिक होती है। यह बीमारी कैसे होती है?इम्यून सिस्टम रीढ़ के जोड़ों पर हमला करता है जिससे लगातार सूजन रहती है। यह सूजन जोड़ों की हड्डियों को आपस में जोड़ने लगती है जिसे Fusion कहते हैं। धीरे-धीरे रीढ़ बांस जैसी सीधी और कठोर हो जाती है जिसे Bamboo Spine कहते हैं।
बीमारी के कारण (Causes)?- HLA-B27 जीन — 90% मरीजों में यह जीन पाया जाता है- अनुवांशिक कारण — परिवार में किसी को हो- इम्यून सिस्टम की खराबी- पर्यावरणीय कारण- आंतों के बैक्टीरिया का असंतुलन- बार-बार संक्रमण
लक्षण (Symptoms)?- पीठ के निचले हिस्से में सुबह अकड़न और दर्द- सुबह उठने पर दर्द अधिक जो व्यायाम से कम हो- रात को दर्द से नींद टूटना- कूल्हे और नितंब में दर्द- गर्दन में दर्द और अकड़न- थकान और कमजोरी- सांस लेने में कठिनाई — पसलियां प्रभावित होने पर- आंखों में लालिमा और दर्द (Uveitis)- एड़ी में दर्द- धीरे-धीरे झुककर चलना महत्वपूर्ण जानकारीएंकिलोजिंग स्पॉन्डिलाइटिस पूरी तरह ठीक नहीं होती लेकिन सही इलाज और नियमित व्यायाम से इसे नियंत्रित किया जा सकता है। इस बीमारी में व्यायाम दवा से अधिक महत्वपूर्ण है। आराम करने से दर्द बढ़ता है और व्यायाम से कम होता है — यह इसकी विशेषता है। क्या खाएं?- ओमेगा 3 युक्त भोजन — मछली, अलसी, अखरोट- हल्दी और अदरक — प्राकृतिक सूजनरोधी- हरी सब्जियां — पालक, ब्रोकली, पत्तागोभी- फल — विशेषकर बेरीज और चेरी- कैल्शियम युक्त भोजन — दूध, दही, तिल- विटामिन D — धूप और मछली- साबुत अनाज, पर्याप्त पानी क्या न खाएं?- प्रोसेस्ड और जंक फूड — सूजन बढ़ाता है- रेड मीट अधिक मात्रा में- शराब- धूम्रपान — बीमारी को तेजी से बढ़ाता है- अधिक नमक- मैदा और रिफाइंड कार्बोहाइड्रेट- तला-भुना खाना- कोल्ड ड्रिंक और सोडा- आराम अधिक करना — व्यायाम न छोड़ें निष्कर्ष (Conclusion)एंकिलोजिंग स्पॉन्डिलाइटिस में नियमित व्यायाम, स्विमिंग और योग सबसे महत्वपूर्ण उपचार हैं। धूम्रपान बंद करना और सही खान-पान बीमारी को आगे बढ़ने से रोकता है। होम्योपैथिक चिकित्सा इस बीमारी में सूजन कम करने और जोड़ों को Fuse होने से रोकने में सहायक है। सकारात्मक दृष्टिकोण और नियमित इलाज से इस बीमारी के मरीज एक सक्रिय और गुणवत्तापूर्ण जीवन जी सकते हैं।

Acute Pancreatitis kis ke vajah se hota hai?
Acute Pancreatitis (एक्यूट पैन्क्रियाटाइटिस) यह बीमारी क्या है?एक्यूट पैन्क्रियाटाइटिस अग्न्याशय (Pancreas) की अचानक आने वाली तीव्र सूजन है। यह एक आपातकालीन स्थिति है जो अचानक शुरू होती है और सही इलाज से कुछ दिनों में ठीक भी हो सकती है। अग्न्याशय वह ग्रंथि है जो पाचन एंजाइम और इंसुलिन बनाती है। जब यह एंजाइम अग्न्याशय के अंदर ही सक्रिय हो जाते हैं, तो वे उसी ग्रंथि को नुकसान पहुंचाने लगते हैं — यही एक्यूट पैन्क्रियाटाइटिस है।यह बीमारी कैसे होती है?सामान्यतः अग्न्याशय के एंजाइम छोटी आंत में जाकर सक्रिय होते हैं। लेकिन जब किसी कारण से ये एंजाइम अग्न्याशय के अंदर ही सक्रिय हो जाते हैं, तो वे अग्न्याशय की अपनी कोशिकाओं को ही पचाने लगते हैं। इससे तीव्र सूजन, दर्द और कभी-कभी अंदरूनी रक्तस्राव भी हो सकता है।
बीमारी के कारण (Causes)पित्त की पथरी (Gallstones) — सबसे सामान्य कारण, पथरी डक्ट को बंद कर देती हैअत्यधिक शराब का सेवन — दूसरा सबसे बड़ा कारणउच्च ट्राइग्लिसराइड स्तर — खून में अत्यधिक वसाकुछ दवाओं का दुष्प्रभाव — जैसे स्टेरॉयड या एंटीबायोटिकपेट पर चोट लगनावायरल संक्रमण — जैसे Mumps वायरसERCP प्रक्रिया के बाद — एक विशेष जांच के दुष्प्रभाव के रूप मेंअनुवांशिक कारणअज्ञात कारण (Idiopathic)
लक्षण (Symptoms)पेट के ऊपरी हिस्से में अचानक तेज और असहनीय दर्ददर्द जो पीठ की तरफ फैलेजी मिचलाना और बार-बार उल्टी होनाबुखार आनापेट को छूने पर तेज दर्द होनापेट फूलना और कठोर हो जानाहृदय गति तेज होनाकुछ गंभीर मामलों में पीलियाकमजोरी और थकानगंभीर मामलों में Blood Pressure कम हो जाना महत्वपूर्ण जानकारीएक्यूट पैन्क्रियाटाइटिस के अधिकांश मामले (लगभग 80%) हल्के होते हैं और कुछ दिनों में ठीक हो जाते हैं। लेकिन 20% मामले गंभीर हो सकते हैं जिनमें अस्पताल में भर्ती होना जरूरी होता है। अगर बार-बार एक्यूट पैन्क्रियाटाइटिस हो तो यह क्रोनिक पैन्क्रियाटाइटिस में बदल सकती है। क्या खाएंबीमारी के शुरुआती दिनों में केवल तरल पदार्थ — पानी, नारियल पानी, हल्का शोरबादलिया और खिचड़ी — जब डॉक्टर ठोस खाना शुरू करने की अनुमति देंउबली हुई सब्जियां — लौकी, तोरई, पालकमूंग दाल का पानी या हल्की दालकेला और सेब — हल्के और सुपाच्य फलपपीता — पाचन में सहायककम वसा वाला दही (थोड़ी मात्रा में)दिन में कई बार थोड़ा-थोड़ा खाएंपर्याप्त पानी और इलेक्ट्रोलाइट्स
क्या न खाएंशराब पूरी तरह बंद करेंतला-भुना और अधिक तेल वाला खानामसालेदार भोजनडेयरी उत्पाद जैसे मक्खन, क्रीम, पनीररेड मीट और फैटी मीटफास्ट फूड और जंक फूडमीठे पेय और कोल्ड ड्रिंककैफीन — चाय और कॉफीएक बार में अधिक खानाधूम्रपान बिल्कुल बंद करें
Videos

Chronic Gastric Ulcer ka homeopathy me ilaj?
१) क्रॉनिक गैस्ट्रिक अल्सर का इलाज?
- क्रॉनिक गैस्ट्रिक अल्सर गंभीर बीमारी है, जिस में पेट की अंदरूनी पर्त में घाव बन जाता है। - जब यह अल्सर लंबे समय तक 3 महीने से भी अधिक बना रहता है. बार-बार वापस आता है, तो इसे “क्रॉनिक” कहा जाता है। - अगर सही समय पर इसका सही इलाज नहीं किया जाए, तो यह गंभीर समस्याओं का कारण हो सकता है.
२) क्रॉनिक गैस्ट्रिक अल्सर के कारण?
- क्रॉनिक गैस्ट्रिक अल्सर कई कारण से हो सकते हैं, जैसे की, - H. pylori बैक्टीरिया के संक्रमण से - बहुत ही ज्यादा मसालेदार तैलीय भोजन करने से - मानसिक तनाव तथा अनियमित जीवनशैली - ये सब कारक पेट के पर्त को नुकसान पहुंचाते हैं, जिस से अल्सर होता है।
३) क्रॉनिक गैस्ट्रिक अल्सर के लक्षण?इस बीमारी के लक्षण इस तरह से हैं, - पेट में जलन होना
- भूख भी सही से नहीं लगना - वजन का कम होना - गंभीर परीस्थिति में खून की उल्टी यह लक्षण दिखाई दें, तो तुरंत डॉ से संपर्क करना चाहिए। ४) क्रॉनिक गैस्ट्रिक अल्सर का सही इलाज?
# 1. दवा के द्वारा इलाज - डॉ. आमतौर पर इस तरह के दवाएं देते हैं: - ओमेप्राजोल, पेट के एसिड को कम करते हैं.
- H. pylori संक्रमण को खत्म करने के लिए एंटीबायोटिक्स
# 2. आहार में परिवर्तन # किन चीजों से बचें - ज्यादा मसालेदार तला हुआ खाना।
- चाय, कोल्ड ड्रिंक्स - शराब तथा धूम्रपान #क्या खाएं - हल्का भोजन- दही , दलिया - हरी सब्जियां तथा फल #3. जीवनशैली में सुधार - धूम्रपान को पुरे तरह से छोड़ दें - शराब को नहीं पीना - नियमित ७-८ घंटे नींद लें
५) क्रॉनिक गैस्ट्रिक अल्सर से बचाव?
- संतुलित आहार को लें - तनाव को कण्ट्रोल में रखे

pancreatitis me sujan hone ka kya ilaj hai?
1) पैंक्रियास की सूजन का इलाज?
- पैंक्रियास (अग्नाशय) मानव शरीर का एक ज़रूरी अंग है, जो पेट के पीछे स्थित होता है। इसका काम पाचन एंजाइम और हार्मोन बनाना है। - जब इस अंग में सूजन आ जाती है, तो इस स्थिति को पैंक्रियाटाइटिस कहते हैं। - यह स्थिति अचानक (एक्यूट) हो सकती है या लंबे समय तक (क्रोनिक) बनी रह सकती है।
2) पैंक्रियास की सूजन के कारण?
- बहुत ज़्यादा शराब पीना - पित्त की पथरी (Gallstones) - ट्राइग्लिसराइड का स्तर ज़्यादा होना - कुछ दवाओं के साइड इफ़ेक्ट - इन्फेक्शन या आनुवंशिक कारण
3) पैंक्रियास की सूजन के लक्षण क्या हैं?
- दर्द भी पीठ तक फ़ैल सकते है.
- जी मिचलाना और उल्टी होना- बुखार; पेट फूलना
4) पैंक्रियास की सूजन का इलाज?
# 1. अस्पताल में भर्ती होना
- अगर सूजन गंभीर है, तो मरीज़ को अस्पताल में भर्ती करने की ज़रूरत होती है।
- नस के ज़रिए (IV) तरल पदार्थ दिए जाते हैं।
- मरीज़ को कुछ समय के लिए बिना खाना दिए रखा जाता है ताकि पैंक्रियास को आराम मिल सके और वह ठीक हो सके। # 2. दवाएँ - डॉक्टर द्वारा बताई गई दवाओं में ये शामिल हो सकती हैं: - दर्द कम करने के लिए पेनकिलर - पाचन एंजाइम सप्लीमेंट
5) घरेलू और प्राकृतिक उपाय?
# 1. हल्का और संतुलित आहार - कम वसा वाला खाना खाएँ
- उबली हुई सब्ज़ियाँ, फल और दलिया खाएँ
- बहुत ज़्यादा तले हुए, चिकनाई वाले और मसालेदार खाने से बचें# 2. खूब पानी पिएँ
# 3. शराब और धूम्रपान से दूर रहें
# 4. नारियल पानी पीने से भी पाचन बेहतर हो सकता है
6) किन चीज़ों से बचना चाहिए?
- बहुत ज़्यादा तेल या घी का सेवन न करें - जंक फ़ूड से बचें
- डॉक्टर से सलाह लिए बिना कोई भी दवा न लें
homeopathy me kidney stones ka ilaj?
१) किडनी स्टोन का इलाज?
- गुर्दे की पथरी बेहद दर्दनाक समस्या है। यह तब होता है, जब मूत्र में रहे हुए खनिज और लवण क्रिस्टल के रूप में जमा हो कर के कठोर पथरी का रूप ले लेते हैं।
- पथरी किडनी में मूत्र मार्ग के कोई भी भाग में बन सकती है। यदि समय पर सही इलाज नहीं किया गया तो यह बेहद गंभीर समस्या हो सकती है.
२) किडनी स्टोन होने के क्या कारण हो सकते है?
किडनी में स्टोन बनने के कई कारण हो सकते हैं, जैसे: की,
- कम पानी को पीने से।
- ज्यादा नमक या तो, प्रोटीन वाला भोजन
- आनुवंशिक के कारण से - कुछ दवा का ज्यादा सेवन करने से
- मूत्र में संक्रमण
३) किडनी स्टोन होने पर क्या लक्षण दिखाई देते है?
- किडनी स्टोन के लक्षण निचे बताये हैं,
- पीठ के निचले भाग में तेज दर्द का होना - पेशाब करते समय जलन का होना। - बार-बार पेशाब करने जाने की इच्छा
४) किडनी स्टोन का सही इलाज क्या है?
# 1. तरल पदार्थ का सेवन करना
- यदि छोटी पथरी है,तो उसका इलाज है ज्यादा से ज्यादा पानी को पीना। - दिन में कम से कम ५-७ गिलास जितना पानी को पीने से पथरी मूत्र के माध्यम से बाहर निकल सकती है।
# 2. दवा से इलाज
डॉ. दर्द को कम करने तथा पथरी को बाहर निकालने के लिए दवा को देते हैं, जैसे की,
- पेन किलर जो के दर्द को कण्ट्रोल करने के लिए।
- यदि संक्रमण हो तो, एंटीबायोटिक्स ५) किडनी स्टोन के लिए घरेलू उपाय?
- घरेलू उपाय से भी किडनी स्टोन को कम करने में मदद करते है,
- नींबू पानी के सेवन करने से पथरी बनने से रोकता है. - तुलसी का रस किडनी को अच्छा बनाये रखने में मदद करता है. -सेब का सिरका पथरी को घुलाने में मदद कर सकता है घरेलू उपाय को अपनाने से पहले डॉ. की सलाह को जरूर लें.
६) बचाव के लिए उपाय?
- डेली उचित पानी को पीना। - नियमित कसरत करना। - समय समय पर अपने स्वास्थ्य की जांच करवाना।
